A Fighting Chance
Published on January 27th, 2021 by Christina Echegaray.
Mary Nicks remembers frantically typing in a Google search from her home in Linden, Tennessee, desperate to find the nearest hospital equipped to care for her twins who were about to arrive far too soon.
Her search for a medical center that could provide intensive care for infants born at 22 weeks of gestation led her to Monroe Carell Jr. Children’s Hospital at Vanderbilt, two hours away in Nashville. She read that the Mildred Stahlman Division of Neonatology at Children’s Hospital is ranked one of the top programs in the nation for the care of critically ill newborns and premature babies. The Level IV NICU was one of the first hospital programs in the world to care specifically for preterm infants, and the Children’s Hospital is the Regional Perinatal Center for Middle Tennessee.
“We were terrified,” Nicks said. “I remember having just a big fear of the unknown. I had an incompetent cervix, and I already knew that I wouldn’t make it to term. I just didn’t know I would deliver my twins as early as I did. When my doctor here confirmed that I was dilated, and they sent me home, I Googled ‘what hospital would try to save a baby at 22 weeks?’”
She and her husband, Cary, began driving toward Nashville.
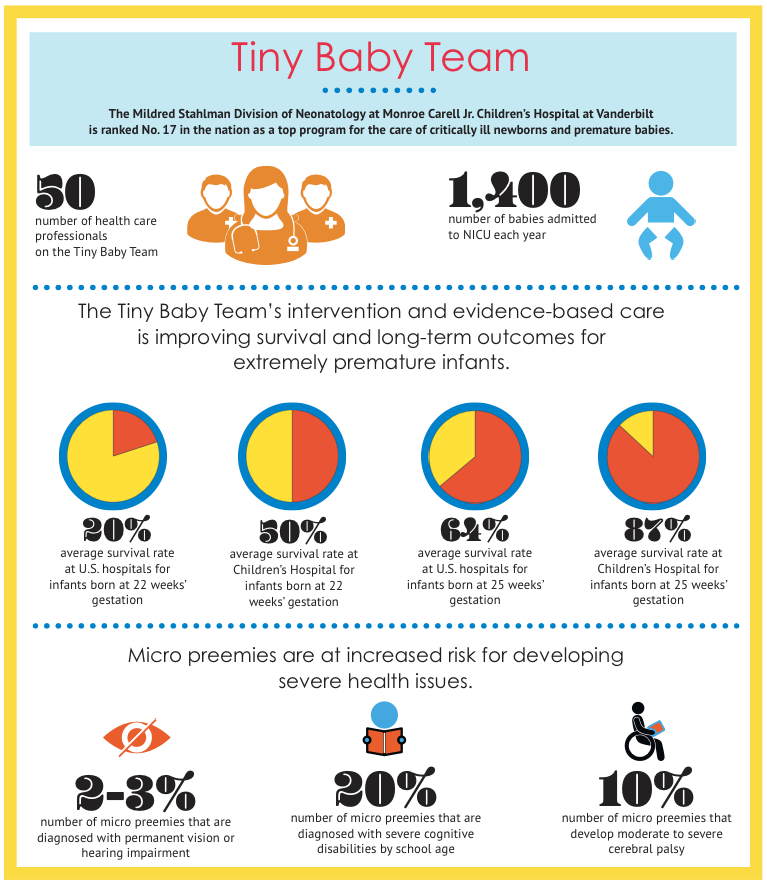
More than 1,400 babies are admitted to the Children’s Hospital’s Neonatal Intensive Care Unit (NICU) each year.
What the Nicks family didn’t learn from that quick internet search is that the hospital also has a specialized Tiny Baby Team to provide the best evidence-based care to improve survival and long-term outcomes for infants born extremely prematurely.
This multidisciplinary group includes approximately 50 health care professionals — physicians, nurse practitioners, nurses, physician assistants, respiratory therapists, occupational therapists, physical therapists, child life specialists, medical receptionists and others — who manage the complex, intensive care of these tiny newborns as well as support and educate their families.
Amazing advances have been made over the past decade in premature infant intensive care, and now the survival rate for infants born in the United States at just 28 weeks is more than 90% with excellent neurological outcomes. However, the survival rate for babies born before 25 weeks’ gestation is lower. And when a baby is born before 23 weeks’ gestation, that survival rate drops dramatically.
The average survival rate at U.S. hospitals for an infant born at 22 weeks’ gestation is less than 20%. At Children’s Hospital, the survival rate for infants born this early at the hospital is now 50%, a significant increase due to the efforts of the Tiny Baby Team. Additionally, the survival rate at Children’s Hospital for infants at 25 weeks’ gestation is 87% and at 24 weeks, survival averages 64%. Unfortunately, if a severely premature infant is born at another hospital and transferred to Children’s Hospital, their survival rate is significantly lower.
“Some pediatric hospitals around the country with centers of excellence dedicated to the care of extremely low gestational age neonates have achieved a 78% survival rate at 22-23 weeks, and that’s why we formed the Tiny Baby Team in the summer of 2019,” said neonatologist Maria Gillam-Krakauer, MD, MEd, the team’s physician leader.
“We have a huge number of people here who are dedicated to improving things for this group of patients and families in Middle Tennessee. There is great humility in these team members as they put aside their individual pride to develop a shared expertise and put patient care and outcomes first. No matter who is on that infant’s care team that day, they get the same, high-quality care.”
Infants born extremely prematurely face a cascade of critical health issues. Severely underdeveloped lungs result in respiratory distress, often requiring at-home oxygen due to chronic lung disease. About 10% of micro preemies develop moderate to severe cerebral palsy. Micro preemies also often have immature digestive systems that lead to poor nutrition absorption as well as the potential for long-term digestive complications. About 20% of micro preemies are diagnosed with severe cognitive disabilities by school age, and another 20% have mild to moderate cognitive problems. Between 2% and 3% of micro preemies have permanent vision or hearing impairment.
Unplanned extubations in preterm infants studied
Unplanned extubations (UEs) in adult and pediatric populations have long been associated with poor clinical outcomes and increased costs to health care systems.Read more »
For nearly a year, the Children’s Hospital Tiny Baby Team pored over published medical studies for the most current research related to the care of extremely premature infants. They used this to develop an evidence-based care strategy designed to protect the babies’ vulnerable neurological systems.
For the first two weeks after birth, the team follows strict care guidelines, including minimal handling to reduce stimulation, carefully positioning the head to reduce the risk of brain bleeds and stringent management of the infants’ fluids and respiration.
“Hands-on care times are scheduled every six hours to allow the babies uninterrupted sleep,” said Jennifer Cortez, RN, nursing lead for the Tiny Baby Team. “Limited stimulation is really what’s important for these little ones. If you do anything that increases their blood pressure even a little bit, it can affect those fragile little blood vessels in their head. A lot of times, bleeding in their head is what leads to just devastating outcomes.”
In addition to very real medical issues, a clinician’s implicit bias might also negatively impact the care of premature infants, Gilliam-Krakauer said. Studies have shown that when providers complete questionnaires related to patients with different ages and conditions, they more often select to offer intensive care to older children and adults with lower survival prognoses over offering intensive care to an extremely premature baby.
“We also see this bias in the language clinicians use to describe premature infants; it’s often not patient-first language,” she said. “It’s hard to understand why this happens, but it’s thought to be because when a baby is born extremely premature, that baby is unable to show personality, wants and desires. This needs to be addressed and requires a reset in the medical community.”
The Tiny Baby Team also hopes to improve communication with community-based hospitals and providers who care for expectant mothers before they arrive at centers specializing in neonatal care such as Children’s Hospital. For example, if an obstetrician believes a woman is likely to deliver prematurely, giving the mother a steroid injection aids maturation of the infant’s lungs and skin as well as reduces the infant’s risk of bleeding in the brain.
“Our referral base is north to Bowling Green and Paducah, east to Cookeville and south to Fayetteville,” Gilliam-Krakauer said. “The challenges we face are delays in transfer of the mother because providers don’t realize that the survival at 22-23 weeks is improving, or failure to give the mother steroids as soon they realize she has preterm labor.”
Over two days as Children’s Hospital clinicians managed Mary’s labor and administered steroids, the Tiny Baby Team also talked to the Nicks about the immediate and long-term prognosis for micro preemies. While the detailed information was appreciated, processing everything was understandably tough, Mary said.
Because of the decreased chance of their twins surviving if delivered at 22 weeks of gestation or of having a good quality of life due to extensive health challenges if they survived, the couple made the hard choice to not take extraordinary measures to save their infants. They told their care team they would hold the babies when they were born and allow them to die naturally.
Then, on Nov. 29, 2019, just 30 minutes before Mary was taken back for an emergency C-section, they changed their minds.
“We were in a really hard spot,” Mary said. “But even with the horrible odds we had been given, we decided we wanted them to try everything they could to save our babies.”
When Cary Nicks Jr. and Adalynn Nicks were born, the Tiny Baby Team immediately began lifesaving care. The infants were struggling through every moment, and their son Cary, seemed to be the sickest.
“We thought we would lose him and not her,” Mary remembered. “They were just so tiny that they couldn’t draw blood samples. When Adalynn passed, it was very sudden. The team was able to run cultures from her to find out what was wrong and use that information to treat Cary. In reality, she saved her brother’s life. Adalynn was his little angel.”
Cortez was caring for Adalynn on the night the twins’ condition quickly deteriorated, and she drew the blood sample that ultimately charted the direction for Cary’s care.
“Often, with tiny babies like these, it’s just the most minute changes in their vital signs that signal something is wrong,” she said. “You see how much these little ones are fighting.”
Adalynn’s test results showed she had developed Escherichia coli (E. coli) sepsis, a blood stream infection. The Tiny Baby Team used this information to quickly intervene with antibiotics for Cary.
As he was fighting this infection in the Neonatal Intensive Care Unit (NICU), Cary also developed necrotizing enterocolitis or NEC, a serious disease that causes infection and damage to the bowel lining. Pediatric surgeon Irving Zamora, MD, MPH, performed emergency surgery to place an abdominal drainage tube.
Over the next five months — during which time a pandemic began — Cary continued to receive intensive care at Children’s Hospital, growing and meeting critical milestones. His parents were also educated by the team about how to feed him, how to position him properly for sleep, warning signs to watch for, and other important caretaking skills for when they returned home.
Cary became the first baby born at 22 weeks who survived since the Tiny Baby Team was formed, a significant milestone for the team, and they are emphatically determined to build on this success.
“This is a story of hope, but it also emphasizes how much work we have to do,” said Gillam-Krakauer. “This shows there can be survival, and there can be good outcomes, even at this very early age. But one of their children died. We were only able to save one of their twins. That shows how much room for improvement we still have.”
When the COVID-19 pandemic began in March 2020, hospital visitation was limited and only one parent could be inside the facility with their son at a time. Thankfully, when Cary was well enough, he was moved into a patient room with a bed for one parent to stay close to him overnight. That made the challenges caused by the pandemic a bit easier, Mary said.
On May 5, members of Tiny Baby Team and the NICU said happy goodbyes to Cary, as his parents settled him in a car seat for the first time and drove home.
And he’s doing well. He turned 1 year old in November 2020, but adjusting for how early he was born, developmentally he’s considered to be 7 months old. Ready to explore everything, he’s beginning to ‘army crawl.’ He’s had two teeth come in, and his once-fragile lungs are doing so well he no longer has to be seen by a pulmonologist.
“By the time we brought him home, he weighed over 9 pounds,” Mary said. “He came home on oxygen, but just three months after being home, we completely weaned him off. As of right now, he just has chronic lung disease and bronchopulmonary dysplasia. And he has some development delays. That’s all.”
Cary recently underwent surgery at Children’s Hospital, again with Zamora, to successfully repair three hernias, and his parents were grateful to already have a strong relationship and connection with the surgeon.

“The Children’s Hospital at Vanderbilt is a great hospital, and that’s why we continue to do most of our care at Vanderbilt,” Mary said. “We trust them, and they were just so wonderful. And we love Dr. Krakauer. She was absolutely amazing, and she always took the time to explain in detail everything that was happening and what we could expect moving forward.”
Although the risks of a negative outcome were extremely high when their twins were born so early, the Nicks said having experts there non-stop to explain everything so they could make informed decisions made them feel empowered. The Tiny Baby Team also gives the family a lot of credit.
“These parents showed tremendous resilience and strength,” Gillam-Krakauer said. “They gave that to him, and that’s why he survived the odds.”
“Every baby is different, but you just have to have faith and take it day by day,” Mary said. “These little miracle babies — they’re strong. Now Cary, our baby, is just a baby. He really has no significant, ongoing problems that will impact his long-term quality of life.”
Hearing about how well Cary and other once-tiny infants are doing gives the Tiny Baby Team affirmation that their efforts are significant and can transform the lives of these families, Cortez said.
“As a team, we’ve had a lot of victories, and we’ve had a lot of losses, too, which is terrible. When you see a baby turn the corner, and there is a positive outcome, it makes it all worthwhile.”
— by Jill Clendening
Hope – Winter 2021