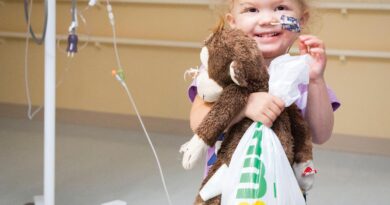
Child-sized care
Published on January 27th, 2015 by user.
A cuddly bear, a friendly smile, a ride in a play car, an ICEE drink, a special bracelet and soft, colorful pajamas are all items that one might find at a child’s sleepover. But at Monroe Carell Jr. Children’s Hospital at Vanderbilt, those are present every day because hospitals don’t have to be, and shouldn’t be, scary for children.
Children’s Hospital provides a unique experience and specialized care from board-certified pediatricians and pediatric specialists, unmatched in Nashville or the region. Children aren’t little adults and shouldn’t be treated as such. They need child-sized doses of anesthesia, colorful rooms and caring faces.
With more than 3,000 procedures performed by the Department of Pediatric Surgery annually in the Rascal Flatts Surgery Center, the highly-skilled surgeons at Children’s Hospital have the expertise to take on a wide range of childhood conditions. Daily, they tackle some of the most common ailments like appendicitis to the more rare and complex cases like tumors and birth defects. And frequently, these surgeons are called into life-threatening situations to perform emergency surgery as part of the trauma team.
“We can do complex trauma cases, congenital pediatric surgery, ECMO, and we take care of some of the most challenging tumors. But we also provide unbelievable services for the more common, ordinary, general surgical problems such as hernia, appendicitis and abscesses,” said Dai Chung, M.D., chair of the Department of Pediatric Surgery and the Janie Robinson and John Moore Lee Professor of Pediatrics. “I am very proud of our faculty and nurses who provide such excellent care. We offer a patient-oriented service and the care we provide is really second to none. Our team does an exceptional job.”
The surgical team, which provides coverage 24 hours a day, includes specialists in pediatric surgery, surgical and pediatric physician trainees, pediatric anesthesiologists and nurse practitioners. The 10 surgeons on faculty have special training in operating on children as well as pre- and post-operative surgical care.
They work with community pediatricians and other specialists to ensure children get the treatments they need.
Below, you’ll read stories of some of the Pediatric Surgery team’s patients and each child’s journey to recovery.
TRAUMA/KENDRA KAUFMAN

Brenda Kaufman held on to her granddaughter, Kendra Kaufman, trying to protect the 6-year-old from rising flood waters until emergency help could arrive.
It had been pouring rain on Sept. 29, 2013, when at 7:29 p.m., in Paducah, Kentucky, their vehicle skidded off the road, went over a 15-foot embankment and plunged into a creek. Brenda Kaufman sustained two dislocated elbows, broken wrists and a broken foot, but managed to hold Kendra above the water. Kendra had visible injuries to her abdomen where the lap belt on her seat belt cut through her skin.
Kira Kaufman, Kendra’s mom, had been waiting for her mother and daughter at home. She happened to be with a volunteer firefighter at the time of the accident, and heard the devastating emergency aid request transmission over the dispatch radio. She rushed to the scene where Kendra and Brenda were rescued and taken to local Kentucky hospitals.
But with severe internal abdominal trauma, Kendra had to be taken by jet plane to Children’s Hospital. LifeFlight had been grounded due to turbulent weather.
The trauma team at Children’s Hospital was ready and waiting for Kendra’s arrival, quickly rushing her to the operating room within minutes.
“I didn’t know what was going to happen to Kendra,” said Kira Kaufman. “I knew she had a big gash and some internal injuries, but they didn’t know exactly what the injuries were yet.”
Pediatric surgeons are often a key component in many trauma cases at Children’s Hospital, being called on as part of a larger team when emergency surgery needs to be performed after a devastating event.
In the operating room, surgeons found that with the force of the impact from the crash, Kendra’s seat belt, while performing its function, had crushed internal organs in her abdomen. The lap belt had compressed the organs against the backbone, said Dai Chung, M.D., chair of the Department of Pediatric Surgery and the interim director of Pediatric Trauma at Children’s Hospital.
“Kendra came to us in a very serious condition. The seat belt tore through the abdominal wall. We knew she didn’t have normal lower extremity neurological function, and a lap belt injury can result in permanent paraplegia,” said Chung, professor of Pediatric Surgery, Pediatrics and Cancer Biology. “These injuries are often very devastating and life threatening. Even after surviving beyond acute injuries, they can lead to lifelong morbidities.”
Chung said the surgical team controlled Kendra’s massive internal bleeding and repaired her abdominal catastrophes, which included mending abdominal wall muscle tears and reconstructing intestinal injuries. After surgery, she went to the Pediatric Intensive Care Unit for eight days, where she was on a ventilator.
Kendra’s prognosis was uncertain. She was alive, but doctors weren’t sure she would walk again because of fractures to the vertebrae with potential permanent spinal cord injury.
But three days post-surgery, the unexpected happened. Kendra moved her legs.
“I was in shock,” her mom said.
Kendra’s recovery was just beginning, however. The road would be long and bumpy. She spent another three weeks in the hospital, before being discharged to a rehabilitation facility in Kentucky, closer to home, where she spent a few more weeks.
“She definitely had her ups and downs. She had her good days and bad days,” said Kira Kaufman.
In a year’s time, Kendra went from not being expected to walk, to scooting on her bottom, then being in a wheelchair, and then to using a walker. Now, she has ankle-foot-orthotics (AFOs) to steady her gait, and she probably won’t need those much longer.
As an active grade-schooler, Kendra, now 7, loves sports and signed up for cheerleading this winter. She wants to return to one of her favorites, T-ball, in the spring.
Chung says Kendra’s story is one of the great successes that Pediatric Surgery, and Children’s Hospital as whole, strive to make happen every day.
“She is one of the many pediatric trauma patients we manage here on a day-to-day basis. Some of the complex injuries we deal with are very challenging. Not every hospital is equipped to provide the comprehensive, quality, tertiary care that our hospital can provide,” said Chung. “That great outcome came in the end for Kendra and her family because of everyone involved, not only in pediatric trauma service, but also in the ICU, pediatric orthopaedics and physical/occupational therapies.”
ROBOTICS/JOSEPH GRAY

Joseph Gray tries to find the humor in any situation, finding ways to make people laugh even when he’s the patient in the hospital.
“It looks like a doughnut, so can I eat it,” Joseph said, joking with nurses about a foam surgical positioning device used to steady a patient’s head during procedures.
“He had the nurses rolling over with laughter,” his mom, Debor’ah Gray said recalling her son’s comedy following an electroencephalogram (EEG) to find out why he was having focal seizures. “He even had the nurses all sign his bed sheet for him.”
The 10-year-old fourth-grader from Murfreesboro, Tennessee, has been in and out of the hospital since he was little. Born with sickle cell disease, a genetic blood disorder that causes pain episodes, he had been sick a lot. When he was 5 years old, doctors at Monroe Carell Jr. Children’s Hospital at Vanderbilt performed a bone marrow transplant, using donor marrow from his older brother Nathaniel, to help Joseph’s sickle cell.
He’s also had an umbilical hernia repaired, and is being tested for obstructive sleep apnea. Through it all he has always been the comedian, Debor’ah Gray says.
But when golf ball-sized gallstones camped out in Joseph Gray’s gallbladder had been causing stomach discomfort for months, it was no laughing matter.
An ultrasound performed at Children’s Hospital confirmed their presence, and he would need his gallbladder removed.
In the Pediatric General and Thoracic Surgery Program, Joseph’s surgeon was able to employ a new innovative approach to removing the gallbladder through a small, single incision using a robotic surgery available only at an elite group of children’s hospitals around the country.
Children’s Hospital was the first in Tennessee to perform a single-site incision robotic cholecystectomy, or gallbladder removal surgery, on a pediatric patient, reducing the number of incision sites for the procedure from four to one.
“I was kind of scared for him to be so young to have his gallbladder removed,” said Debor’ah Gray.
“He stayed overnight because they wanted to monitor him since he had been a stem cell transplant patient to treat sickle cell five years ago. But within two days he was up and running around, being a normal kid. He didn’t even want any more pain medicine.”
Dai Chung, M.D., Janie Robinson and John Moore Lee Professor of Pediatrics and chair of the Department of Pediatric Surgery, performed Joseph’s surgery.
He said because Joseph had a small surgical scar from a previous umbilical hernia repair, he was able to perform the gallbladder removal operation via the same small single incision, thereby avoiding multiple additional surgical incisions.
“The single-site robotic surgery uses a single 2.5 cm in diameter trocar (incision) via an infraumbilical approach. Using these specially designed tools for the robot, we were able to perform the cholecystectomy on Joseph through one very small incision,” Chung said.
“Joseph was an ideal patient. Since then, he has been completely relieved of the worsening symptoms he experienced and returned to his normal activities in no time.”
Gallbladder removal surgery is becoming more common, in part because of increasing childhood obesity, Chung said, though Joseph did not fall into that category.
Children’s Hospital first began using the cutting-edge robotic device to perform minimally invasive pediatric surgeries in 2011. The first procedure performed was to repair a kidney blockage in an 8-year-old girl.
Now, surgeons are performing even more minimally invasive surgeries for specific conditions with this single-incision procedure.
The robot unites conventional laparoscopy and traditional open surgery, though at a more advanced level. A surgeon sits at a console directing the tool’s four arms, conducting delicate procedures with precise movements.
Potential benefits can include minimal scarring and a shortened recovery period. Children’s Hospital surgeons who use the device have had extensive training.
“As the robotic surgical community gains more experience and expands this approach for other surgical conditions, we’re in a prime position to lead the rest of the field. We’re at the forefront of this cutting-edge technology,” Chung said.
Joseph’s mother said he has been symptom-free since his surgery. He’s back to riding his bike, shooting hoops outside and doing his favorite thing, making people laugh. “You can’t even really see the scar,” she said.
ECMO/EASTON CUNNINGHAM

Easton Cunningham is a rambunctious 2-year-old who loves toy cars, balls and running.
“He likes to run and run—non-stop,” chuckles his mom, Kerry Cunningham, with emphasis on “non-stop.”
But for his first month of life, Easton’s parents, Kerry and Chad, weren’t sure they would ever get to enjoy his energy and enthusiasm for life. During birth at a local hospital, Easton inhaled meconium (a newborn’s excrement) while still in the womb and was suffocating. His mom had an emergency cesarean section. Easton couldn’t breathe and needed nitric oxide, not available at the hospital where he was born.
Given the choice of a hospital, the Cunninghams, who live in Murfreesboro, Tennessee, wanted Easton transported to Monroe Carell Jr. Children’s Hospital at Vanderbilt.
“He was swollen and blue. It’s probably one of the scariest things I had ever seen,” Kerry said.
After several days of ups and down and oxygen support, Easton’s lungs weren’t performing well enough. But he was in the right place to get the care he so desperately needed. He was placed on extracorporeal membrane oxygenation (ECMO)—a life-support system that oxygenates the blood through a machine that then returns the oxygenated blood back into the body either through the arteries or veins.
The mobile machine is used both in and outside the operating room and can support vital heart and lung function for weeks at a time until the organs can recover, or sometimes until a heart transplant is available.
Since 1989, an estimated 955 patients, infants, children and adults, have had ECMO support at Vanderbilt. The ECMO program celebrated its 25th anniversary in November with a reunion of about 250 former patients and their families.
The ECMO program at Children’s Hospital is one of the largest and most successful in the country. For the past seven years, it has received recognitions as a Center of Excellence from the international consortium Extracorporeal Life Support Organization (ELSO), earning the ELSO Award for Excellence in Life Support.
The award is given to programs that show a commitment to exceptional patient care, and have a high level of quality standards including specialized equipment and supplies, defined patient protocols and advanced education of all staff members.
Asked what makes the ECMO program at Children’s Hospital so successful, John Pietsch, M.D., replied simply: “the people.”
“We’ve got a great team. It’s truly a team—we have neonatology, pediatric intensive care, the pediatric cardiac team, adult trauma team, adult intensive care, who work closely with the ECMO team, not to mention all the nurses and the respiratory therapists and everyone else. It works because we’ve got all these people working together,” said Pietsch, surgical director and founder of the ECMO program at Vanderbilt. “The equipment has also gotten better and we know which patients ECMO is best for.”
Pietsch arrived at Vanderbilt in 1986 from Louisville, Kentucky, where he had been a part of an ECMO team. He convinced Vanderbilt to start an ECMO program, and prepared for the right child to be the first patient. That patient, Chelsea Brown, arrived at Vanderbilt Nov. 24, 1989, and was the first ECMO patient at Vanderbilt and in Tennessee. Like Easton, she had inhaled meconium and was unable to breathe. Today, she is 25 years old and is a college graduate living in Boston.
For Pietsch, the reunions are a defining moment in which he gets to see the results of his team’s work.
“You get to see patients you haven’t seen for some time. It’s very satisfying for us to see all the successes,” he said.
Easton Cunningham is one of those successes. He was on ECMO for five days.
“The ECMO techs were all wonderful and the ECMO nurses were great. I cannot say enough about the employees there,” Kerry said.
The Cunninghams got to bring Easton home on March 1, 2013, when he was about 6 weeks old, and he has done well since.
“He is pretty typical. He has surpassed all his developmental goals and he’s just typical all boy,” Kerry said.
– by Christina Echegaray