Next-Level Care
Published on August 30th, 2021 by Jessica Pasley.
For the first 18 months of his life, Carter Ray lived at Monroe Carell Jr. Children’s Hospital at Vanderbilt.
After several innovative, minimally invasive surgical techniques used over a year to improve his health — including a first-of-its-kind procedure performed in the United States — Carter finally went home, to Lynchburg, Tennessee.
Minimally invasive surgery (MIS) is exactly what it sounds like — the least intrusive pathway to performing a wide range of medical procedures and surgeries. This allows children to recuperate faster and with less pain.
The innovative technique allows a surgeon to use telescopes and operating instruments through small incisions. Surgeons at Children’s Hospital have extensive experience and expertise in MIS, which has been performed at Children’s Hospital since the 1990s.
Depending on the type of surgery, there are several minimally invasive surgical methods that may be utilized (robot-assisted surgery, laparoscopy, endoscopy, arthroscopy, bronchoscopy, gastroscopy, among others) across many pediatric specialties.
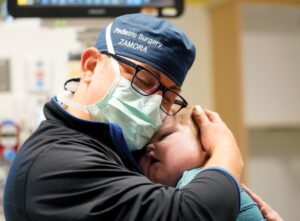
“We have a fantastic group of surgeons who have been doing this for a very long time,” said Irving J. Zamora, MD, MPH, assistant professor of Pediatric Surgery and director of Advanced Minimally Invasive Surgery. “It continues to evolve, and we are learning more advanced technology and approaches to offer our patients.
“We are building a program that is allowing us to do high-level, advanced surgical operations and meet the needs of some of the most critically ill, medically complex patients, like Carter.”
First-ever use in the U.S.
Carter, born Nov. 3, 2019, was diagnosed with a very rare form of esophageal atresia (EA), transesophageal fistula (TEF) Type B and tracheobronchomalacia (TBM), conditions that ultimately required reconstruction of the esophagus to allow secretions and nutrients to reach his stomach.
Seen in 1 in 4,000 U.S. births, EA is a rare birth defect where part of the esophagus isn’t developed properly and sometimes has a connection to the airway. TEF caused secretions to collect into Carter’s airway and lungs and led to several bouts of pneumonia, while TBM resulted in excessive weakness and near collapse of his windpipe wall. These conditions interfere with breathing and can cause significant lung issues.
The complexity of the case required the specialized care of a surgical team at Children’s Hospital, led by Zamora, who put together a group of experts including surgery partners Harold Lovvorn, MD, and Nathan Novotny, MD, as well as colleagues from Otolaryngology-Head and Neck Surgery, Christopher Wootten, MD, and Lyndy Wilcox, MD.
Together, they focused on repairing the esophagus and airway using minimally invasive surgery techniques — all with the ultimate goal of getting Carter home.
What would have been a potentially daylong, high-risk, open-chest and abdominal surgery was shortened to a 38-minute endoscopic procedure.
The multidisciplinary team focused on repairing Carter’s esophagus and airway, which required the use of special magnets to connect the two ends of a congenitally separated esophagus. Zamora collaborated with Michael Harrison, MD, and a team at University of California San Francisco (creators of the magnet device) and Oliver Muensterer, MD, PhD, in Munich, Germany (the only other surgeon in the world to use the magnets).
Given the novel nature of this approach, the procedure required a compassionate use approval from the Food and Drug Administration. The team spent months preparing for the first use of the Connect EA – Magnamosis device in the U.S.
“Not many institutions are doing this, and even fewer are using a minimally invasive surgery approach to perform these innovative procedures,” said Zamora. “While this was a milestone for the institution and others interested in such innovations, most importantly, we saved Carter’s life.”
Small incisions, big impact
One of the surgeons partnering with Zamora on Carter’s care, Christopher Wootten, MD, associate professor and chief of Pediatric Otolaryngology-Head and Neck Surgery, has long used minimally invasive surgical techniques in his practice.
In addition to extensive use in the airway, Wootten uses MIS for procedures including endoscopic ear surgery and tympanoplasty (repair to the eardrum). The practice has allowed for better outcomes and reduction in the number of incisions or need to drill behind the ear for access, which ultimately lessens the chance of postoperative complications.
“We have a fairly large patient population with congenital anomalies,” said Wootten. “Having the ability to work in very small spaces has enhanced our ability to perform very intricate procedures that are difficult to do microscopically.”
Wootten’s team has several goals for the use of minimally invasive approaches, which include repairing abnormalities of the skull base; enhancing cochlear implants; and eventually managing disorders of the eustachian tube.
“Over time, we have been able to enhance our reputation through the creation of the endoscopic ear course, which is a CME (continuing medical education) offering,” said Wootten. “It’s brought us national attention. This course holds professional importance and shows people on the national level that we have become experts. They learn from us and take these novel techniques to their patients all over the country.”
MIS also serves as an invaluable teaching tool, allowing images to be viewed on giant screens (both live and recorded) to better instruct future surgeons.
Children’s Hospital offers MIS for a wide range of complex conditions with the goal of providing equal or superior clinical outcomes as well as reducing surgical risks, use of pain medications and hospital length of stay.
3D models aid precision image-guided surgery
To assist with providing optimal surgical views, the hospital offers a unique opportunity to the surgeon: 3D images of the anatomy.
Sumit Pruthi, MD, professor of Radiology and Radiological Sciences and Pediatrics and chief of Pediatric Neuroradiology, spearheaded and led the establishment of the 3D Printing Center to assist with both pediatric and adult cases.
Begun in 2016, the program has grown in capacity and scope, recently adding a Stratasys J735 printer, which allows for the creation of highly complex models.
A print or 3D model may require between two to 24 hours to complete, depending on complexity, and typically uses multiple materials, colors and textures for a more lifelike replica of the internal structure of the patient.
“Better information leads to better outcomes,” said Pruthi. “Having the ability to hold the model to manipulate, turn and study in a three-dimensional space, allows the surgeons and teams to conceptualize and develop a strategy on how best to treat patients.
“While most of the anatomy can be seen using two-dimensional imaging, the model affords the ability to see the anatomy from multiple angles and perspectives, giving the surgical team a greater advantage,” he said.
Since the creation of the 3D Printing Center, approximately 825 models have been printed to assist in decision-making and serve as a practice tool prior to surgery. In some cases, the models have helped to detect other abnormalities, and in others, have prompted teams to review additional approaches to a procedure because of what they see.
The model also plays a role in medical education/ teaching for both residents and parents.
“Another piece of this is sharing images depicting their child’s anatomy and the surgical procedure with the parents,” said Pruthi. “Patients’ families appreciate our models as their physicians walk them through the surgical process. I can only imagine how difficult it can be to try to comprehend what the teams are saying when a parent is focused on their child; our images help the parents direct their attention to the procedure being described.”
Areas utilizing the innovative printing technology include craniofacial, orthopaedics, cardiology, cardiothoracic surgery, ENT, urology, gastroenterology, oncology and pediatric surgery.
According to Harold Lovvorn III, MD, professor of Pediatric Surgery and medical director of Pediatric Trauma at Children’s Hospital, the 3D images make understanding the anatomy more accurate, resulting in a safer procedure for the patient.
“The use of image-guided tools will allow us to extend the MIS program to more challenging conditions,” said Lovvorn.
While every condition is not suitable for MIS, the ever-growing list of diagnostic and therapeutic uses and rapidly expanding programs offers a glimpse into the future of medicine for pediatric patients.
MIS has revolutionized many surgery techniques in both chest and abdominal procedures and is more commonly becoming the standard approach for many of the conditions treated at Children’s Hospital, proving that the smallest of incisions have a big impact.
“Our commitment is to provide the latest technologies and innovative tools when performing surgery on children, whether for birth anomalies, tumors or trauma,” said Lovvorn.
Within this age of innovation, the patient is the ultimate winner as the newest techniques provide multiple benefits, including: less pain and the use of fewer opioids; shorter recovery and hospital stays; and the ability to stay on track with continued treatments in the case of cancer therapies.
“Although we tout and marvel at all the innovation that minimally invasive surgery offers in the surgical care of children and newborns, when you get right down to what’s most important, we ultimately are doing what is best for our patients,” he said. “We want our patients and their families to be able to return to their normal activities sooner rather than later.”
A chance for many firsts
Carter went home for the first time on April 27, where he joined his big brother, Jackson, 3.
“It’s not like this has been easy, and we have all had to take risks, but without them, we wouldn’t have learned how to repair his esophagus,” said his mom, Lacey Ray. “Sometimes you have to take chances to make improvements, and you have to have someone willing to be the first.”
Although tracheostomy- and ventilator-dependent, Carter, now 21 months old, no longer requires tubes coming from his mouth and nose to suction secretions and help him breathe.
With the help of physical and occupational therapy, the team is hopeful that he will learn to swallow, walk and begin experiencing many firsts.
“We are all home together, and he loves being here,” said Lacey Ray. “He has come out of his shell. He is smiling a lot, laughing and even rolls to his belly,” she said, giving credit to Zamora and his team. “I’m glad there are teaching hospitals like this. It’s why they can try new things that will hopefully help others in the future who will need this kind of procedure.
“I’ve heard people say that once a child comes home, they thrive. It is so true. He is a miracle, and we are looking forward to our future together.”




