Play On
Published on July 6th, 2023 by Nancy Humphrey.
Two-year-old Ramsey Crawford holds the hand of her physical therapist in the hallway outside her room at Monroe Carell Jr. Children’s Hospital at Vanderbilt as they work to strengthen the toddler’s wobbly legs.
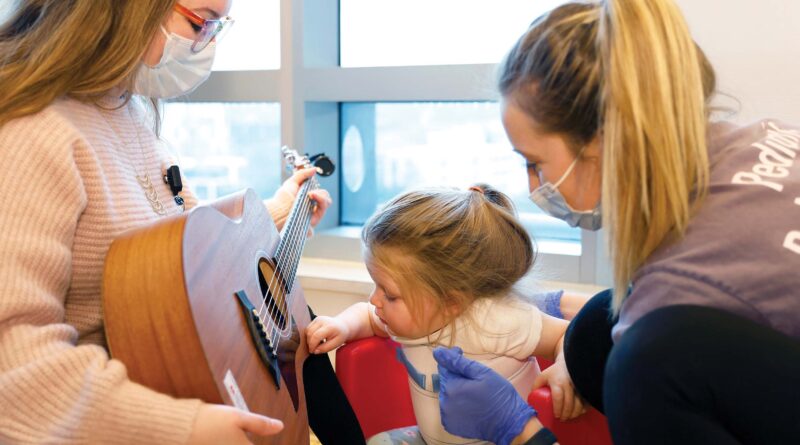
Ahead of pony-tailed Ramsey, scooting backward on her knees, is Jess Knoble, MT-BC, one of Monroe Carell’s three board-certified music therapists. She’s strumming a guitar and singing to the beat of Ramsey’s steps, “The ants go marching one by one, hurrah, hurrah.” When Ramsey changes her tempo, so does Knoble, modifying the words from the Disney song “Let it go” to “Ramsey, go, Ramsey, go.”
On Christmas Day 2022, when Ramsey’s parents were unable to awaken her, they rushed her to the hospital in their hometown of Bowling Green, Kentucky. She was diagnosed with ADEM (acute disseminated encephalomyelitis), a rare neurological disorder in which the immune system causes an intense attack on the brain, and sometimes the spinal cord and optic nerve. It often results in loss of vision in one or both eyes due to inflammation of the optic nerve; weakness that can be severe; and difficulty coordinating intended movement, such as walking.
“We didn’t think she’d ever be OK,” said her father, Benjamin Crawford. “She’s truly a miracle. We were prepared for the worst but are praying for the best. She’s come a long way,” he said, watching Ramsey working with Knoble. “Music therapy is the highlight of her day.”
Music therapists work with children and their families across inpatient areas at Monroe Carell, using music in unique ways with each child to help with chronic pain, physical rehabilitation, psychiatric symptoms, end of life, procedural support and coping with hospitalization and disease. They are part of the medical team supporting the whole patient, using evidence-based music interventions to provide individualized care for each patient’s medical diagnosis, course of treatment and discharge timeline.
Knoble sits on the floor with Ramsey, maneuvering a flat electronic drum pad so that Ramsey is encouraged to use her weak side to play. After she tires of the drums, she blows into a slide whistle that is used to improve her respiratory strength. Everything is with a specific goal in mind — to help Ramsey gain strength.
“We’re not just playing and having fun. We are (having fun), but with our clinical training, we’re using things we have in our toolbox to make it a fun environment where kids want to engage,” said Knoble, who has additional training in neurologic music therapy.
“What I’m doing (while Ramsey walks) is called rhythmic auditory stimulation,” Knoble explains. “Everybody has a natural rhythm within themselves; it’s called entrainment. We naturally want to latch on to an external beat. It’s why we tap our foot to a song, why we bob our head to a beat. Our body wants to latch on to this external factor.”
Established in 2005 by Tom and Maria Fouce through the Julian T. Fouce Fund, Monroe Carell’s music therapy program was developed in memory of their son, Julian, a great lover of music who died that year.
“They saw the impact and the benefit. They have been really passionate about watching the program grow, and we’ve been fortunate that they’ve continued to stay involved,” said Dana Kim, MT-BC, a board-certified music therapist at Monroe Carell. “We’re grateful for all they have done.”
Music therapy techniques are backed by research showing how they can best assist children during hospitalization.
The hospital’s music therapists have bachelor’s and master’s degrees in music therapy, over 1,200 clinical hours, and have passed a national exam administered by the certification board for music therapists.
“The music therapy program has become a staple in our menu of care for children and families at Monroe Carell,” said Janet Cross, MEd, CCLS, CPXP, senior director, Patient- and Family-Centered Care. “The Fouce family had a wonderful vision in 2005, and we are able to continue to grow the program to meet that vision with their support. The role that the music therapists play in the care for hospitalized children is so very important. They are able to connect in even the most stressful situations and provide excellent support for children and families.”
Anyone on a child’s care team can place an order for music therapy, or it can be requested by the family. It starts with a look at the medical record, then the therapists perform an assessment to see how the patient and family respond. There’s a strong focus on building a relationship with the patient.
“Everything we’re doing, we’re trying to do as equals on a playing field,” Knoble said. “Rather than just coming in and playing the guitar, maybe we’re talking to the patient and seeing if they’re having difficulty with being able to relax. We discuss and figure out what music they listen to. We assess if playing the guitar live will be helpful. Rather than us just determining what music might be best, we figure out with them what’s going to work well for them.”
Music therapy might not be the right fit for every child, says Kim.
“It’s very individualized. That’s why we work so closely with our other colleagues. Perhaps spiritual care is really what this family needs or something else our child life colleagues have to offer. That’s why the assessment is so important. Kids and families can always tell us no and empower that choice making. Maybe it’s not right for this hospitalization, but it might be on down the road,” Kim said.
To participate in music therapy, patients don’t have to be musically inclined.
“Sometimes children and families who don’t have that experience and have never utilized music in that way are the ones that can benefit the most,” Kim said.
Ryan Neighbors, 13, from Louisville, Kentucky, has spina bifida and was at Monroe Carell in February for an extended stay as she recovered from traction surgery and a spinal fusion for her scoliosis.

Ryan, who is outgoing, loves music and missed her friends, met often with Kim, as they worked on developmental goals and self-expression, including songwriting.
With Kim’s help, Ryan wrote a song about the excitement she’s feeling about finally getting a golden retriever service dog. She has waited several years for her canine companion and hopes to get it this year.
After talking for a few minutes during a visit, Kim played guitar while Ryan used a bejeweled microphone to sing one of her favorite songs, “Shake It Off.” Then, she practiced singing the song about her dog.
Ryan’s mom, Shelly King, said music therapy has helped her daughter cope during the long hospital stay. “Music therapy has helped her learn how to meditate and calm down when she’s anxious. It helps her get creative and take her mind off things going on medically.”
Kim said teenagers in the hospital can have a rough time being isolated from their friends and may withdraw during their time in the hospital.
“Music in the hospital is so important for them. It’s an important outlet for expression, for identity and for coping throughout the hospitalization,” she said. “It can also help build confidence and empower adolescents to actively participate in their health care.”